Dr. Tony Lam, (L), is a Senior Scientist at Toronto General Hospital Research Institute, and Dr. Song-Yang Zhang is a postdoctoral researcher in his lab. (Photo: UHN StRIDe Team)
Researchers at the Toronto General Hospital Research Institute (TGHRI) have discovered that the drug metformin acts through the kidney to lower weight and treat obesity.
Metformin is the first-line medication for the treatment of obesity-associated Type 2 diabetes and has been in use for close to 30 years to lower blood sugar levels. It has also been documented to cause weight loss; however, exactly how it mediates weight loss was uncertain until now.
“We knew from previous studies that metformin increases the blood levels of a messenger molecule – the GDF15 protein – which acts in the brain to decrease hunger,” says Dr. Tony Lam, Senior Scientist at TGHRI and senior author of the study. “However, before this study, we did not know which organ helped metformin to do this.”
“Understanding the way in which metformin acts is key to understanding how food intake and body weight are controlled in the body,” says Dr. Song-Yang Zhang, postdoctoral researcher in the lab of Dr. Lam and first author of the study.
To find out how metformin mediates weight loss, Dr. Lam’s team referred to the literature to identify the organs that express the GDF15 protein – namely, the upper small intestine, ileum and kidneys. They then prevented the synthesis of GDF15 in these organs, one at a time, and tested whether treatment with metformin increased GDF15 levels in the blood (along with the expected reductions in food intake and body weight).
“When we started working on this, we hypothesized that the small intestine would be responsible for the ability of metformin to induce weight loss,” explains Dr. Zhang. “This is because metformin works through the intestine to elicit changes in blood sugar and why it’s such an effective therapy for diabetes.
“However, our experiments proved our hypothesis to be wrong. In experimental models, when we prevented the small intestine from secreting GDF15, we still saw GDF15 levels spike in the blood as well as the lowering of food intake and weight in response to metformin.
“Only when we blocked GDF15 production in the kidney were we able to shut down GDF15 levels in the blood and cancel the effects on food intake and weight.”
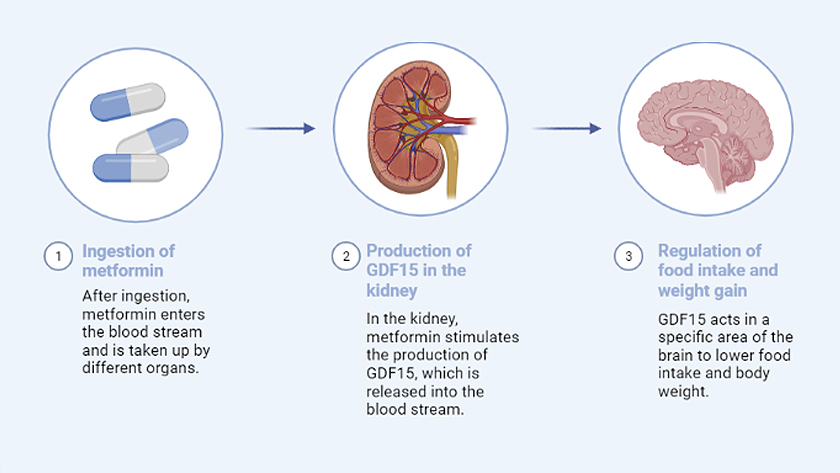
These findings reveal that the kidney is involved in regulating energy balance in the body.
“Along with regulating blood pressure, erythropoiesis, and bone mineralization, our study adds to the known roles of kidney,” concludes Dr. Lam, who also holds a Tier 1 Canada Research Chair in Diabetes and Obesity at TGHRI and the University of Toronto. “By implicating the kidney in weight loss, this work also lays the foundation for new, more targeted therapies to address the obesity epidemic.”
In addition to using experimental models, the researchers collaborated with nephrologists Drs. Heather Reich and David Cherney from UHN, as well as Laura Mariani from the University of Michigan, to conduct experiments using existing human clinical data.
To do this, they analyzed the levels of GDF15 in 360 human kidney biopsies and found some correlation with the levels of GDF15 in the blood of patients. While preliminary, these findings support the idea that GDF15 originating from the kidney contributes to blood levels of the protein.
“In order to translate these findings to the clinic and help patients, we have launched the Diabetes Obesity Initiative at TGHRI,” says Dr. Lam. “This collaborative framework enables researchers, clinical investigators, nephrologists and other experts to come together to discuss ideas and test hypotheses both in the lab and the clinic.
“Knowing that metformin acts through the kidney opens new and exciting avenues for the development of treatments for obesity and the debilitating and devastating conditions that come with it.”


