Candice Cruise found out at 22 weeks of pregnancy that she had a deadly condition called pulmonary hypertension, but a multidisciplinary team came up with an ingenious plan to save her and the baby. (Photo: UHN)
Candice Cruise was 22 weeks pregnant when, coming back home one day with her husband Collin, she noticed on the car’s sun visor mirror that her lips had turned blue. She had been feeling a bit out of breath on recent days, but had dismissed it as something common during pregnancy.
The couple decided to go to the local hospital and get Candice checked.
“It all happened so fast. When I look back, it scares me to think what would have happened if we didn’t seek help that day,” says Candice.
Candice and Collin could never imagine the journey they were about to embark. For over four months, 140 kilometres away from home, they went through an emotional roller-coaster which took them from fighting a deadly condition for mother and baby, being supported by a world-first innovation, open-chest surgeries, pre-term delivery, lung transplant, and finally back home with a happy ending – mother and baby safe, healthy.
But it was indeed a long journey.
When Candice arrived at her local hospital with blue lips back in April, her oxygenation was so low that the doctors quickly decided to transfer her to Toronto’s Sinai Health System – the reference centre for high-risk obstetrics.
Shortly after arriving there, the medical team then made the call to transfer Candice to University Health Network’s (UHN) Toronto General Hospital for evaluation of a possible devastating heart-lung condition known as pulmonary hypertension. UHN has a comprehensive pulmonary hypertension program and is the provincial lead for extracorporeal membrane oxygenation (ECMO) – a last resource for patients with acute respiratory and circulatory failures.
After confirming the diagnosis of pulmonary hypertension, her condition began to become unstable. A quick decision was required to stabilize her and she was placed on ECMO.
“At that time, doctors told us unfortunately that the safest would be to terminate the pregnancy to keep Candice alive,” Collin recalls.
However, as Candice stabilized in the hours and days that followed, medical leads from different specialties at UHN, with support from Sinai Health and The Hospital for Sick Children (SickKids), started to ask themselves if anything could be done to save both, mother and baby.
“I could feel the baby moving inside me, so strong. I knew there was nothing wrong with him, and I felt he had a good chance,” says Candice.
“I wasn’t ready to give up.”
A life-threatening condition
Candice had a condition called pulmonary hypertension, a life-threatening disorder that leads to the narrowing of the arteries in the lungs. This narrowing makes it difficult for the right side of the heart to pump blood through the lungs, which eventually causes the heart muscle to become weak and fail.
The condition is especially dangerous during pregnancy, since the growing baby puts additional stress on the mother’s circulatory system.
“We had never seen a case like this. Pulmonary hypertension is a dangerous condition, even more so for pregnant women, with a high risk of death for both mother and fetus,” says Dr. John Granton, respirologist, intensive care physician and Director of the Pulmonary Hypertension Program at UHN.
Most experts recommend that patients with pulmonary hypertension avoid pregnancy given the high risk of death for the mother and her baby. However, Candice was unaware of her condition before she reached 22 weeks of pregnancy.
“Our teams in Respirology, Cardiology, Surgery, Intensive Care, all put their heads together to find a solution and save this mother and baby,” says Dr. Shaf Keshavjee, Surgeon-in-Chief of UHN’s Sprott Department of Surgery and Director of the Toronto Lung Transplant Program at UHN’s Ajmera Transplant Centre. “This case is a real testament to how far medical advances and team work can go. It is a true medical miracle.”
An ingenious plan
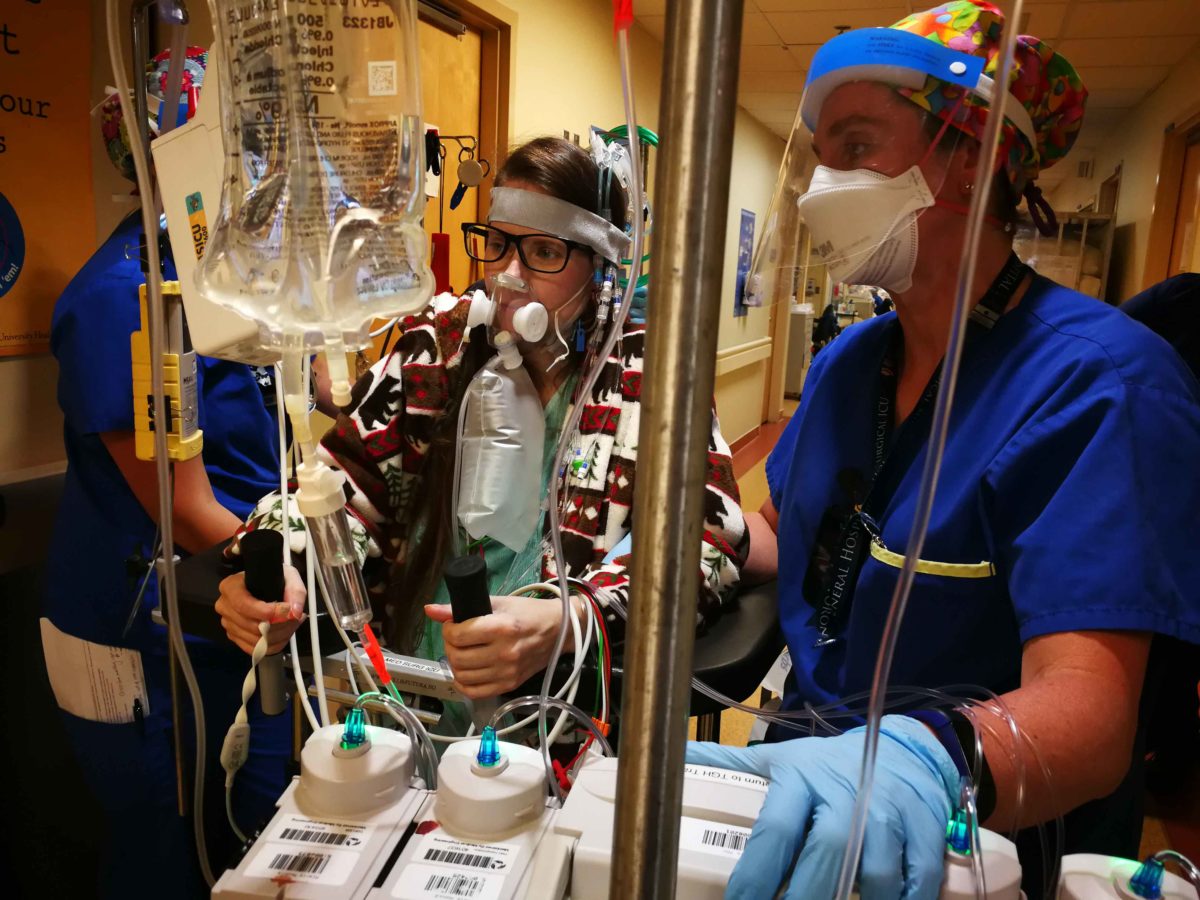
Experts from different programs at UHN, including Respirology, Cardiology at the Peter Munk Cardiac Centre, Intensive Care, Anaesthesiology, Sprott Department of Surgery and Ajmera Transplant Centre, with support from Obstetrics at Sinai Health and Neonatal care at SickKids, developed an ingenious plan to keep Candice stable and buy her pregnancy a few more weeks, to give the developing baby the best chance at life.
The solution was to use an adaptable extracorporeal membrane oxygenation (ECMO) system called Novalung – a low resistance membrane that works as an external artificial lung, able to support the heart while also allowing it to continue to pump. Donors to UHN Foundation have generously supported the acquisition of life-saving ECMO technology.
“That was never done before anywhere in the world,” says Dr. Keshavjee.
The system adapted to Candice’s needs as her pregnancy progressed for the following six weeks.
There were, however, complications along the way. Candice required close monitoring, adjustments to the ECMO settings and some surgical interventions.
“We had to operate on her a few times, and several bed-side interventions to make sure she was stable enough,” says Dr. Laura Donahoe, the thoracic surgeon with UHN’s Sprott Department of Surgery looking after Candice.
“As this was a world-first, we didn’t have any literature to guide us. We had to use all the expertise of our teams to make clinical decisions that we hoped would achieve the best possible outcome.”
The partnership with Sinai Health – the lead hospital in high-risk obstetrics – was key to push the envelope and provide Candice the best possible care.
“In a complex case like Candice’s, difficult choices need to be made that balance the risks to the mother with the health of the developing baby,” says Dr. John Snelgrove, maternal-fetal medicine obstetrician at Sinai Health who supported Candice’s care.
“The NovaLung presented a novel strategy to support Candice’s heart long enough to carry her pregnancy into the third trimester. This is a remarkable medical success, but by far the most amazing part of this story is how courageously Candice persevered, and how dependably Collin supported her during those challenging weeks,” he adds.
Delivery
At 28 weeks and six days, Candice remembers the moment she and her care team decided it was time.
“It was getting very hard to breathe as the baby was pushing my diaphragm. It was too much, plus all the tubes coming out of me.”
Candice was going to be taken to the operating room at Toronto General Hospital for her C-section – something extremely rare as the hospital does not have an Obstetrics Department. But Candice needed to be fully monitored by ECMO experts during her delivery, as she was still being supported by the artificial lung system.
A multidisciplinary team from UHN, Sinai Health and Sick Kids came together to support this high-risk C-section.
“It was so inspiring to see doctors, nurses, and respiratory therapists from these three hospitals come together on such short notice and work cooperatively as one big team. Everybody in the OR played a vital role in the safety of Candice and her baby that day,” remembers Dr. Snelgrove.
Candice had to undergo a general anaesthetic for the C-section, as the team was worried that she would become very unstable during this time and require an increased level of ECMO support. The team prepared Candice for the possibility that they would have to open her chest in order to support her heart through the increased stress of the C-section, which would mean that she would be asleep for at least the first few days of her son’s life.
With excellent anaesthesic care, and the ECMO team prepped and ready, the delivery went smoothly and the heart surgery wasn’t needed. The doctors woke Candice up and she was able to meet her son Cameron in the OR.
“It was like a dream. I was expecting to be out for a few days, so I was confused at first, but it was so amazing,” says Candice.
“It was a really special moment,” echoes Collin.
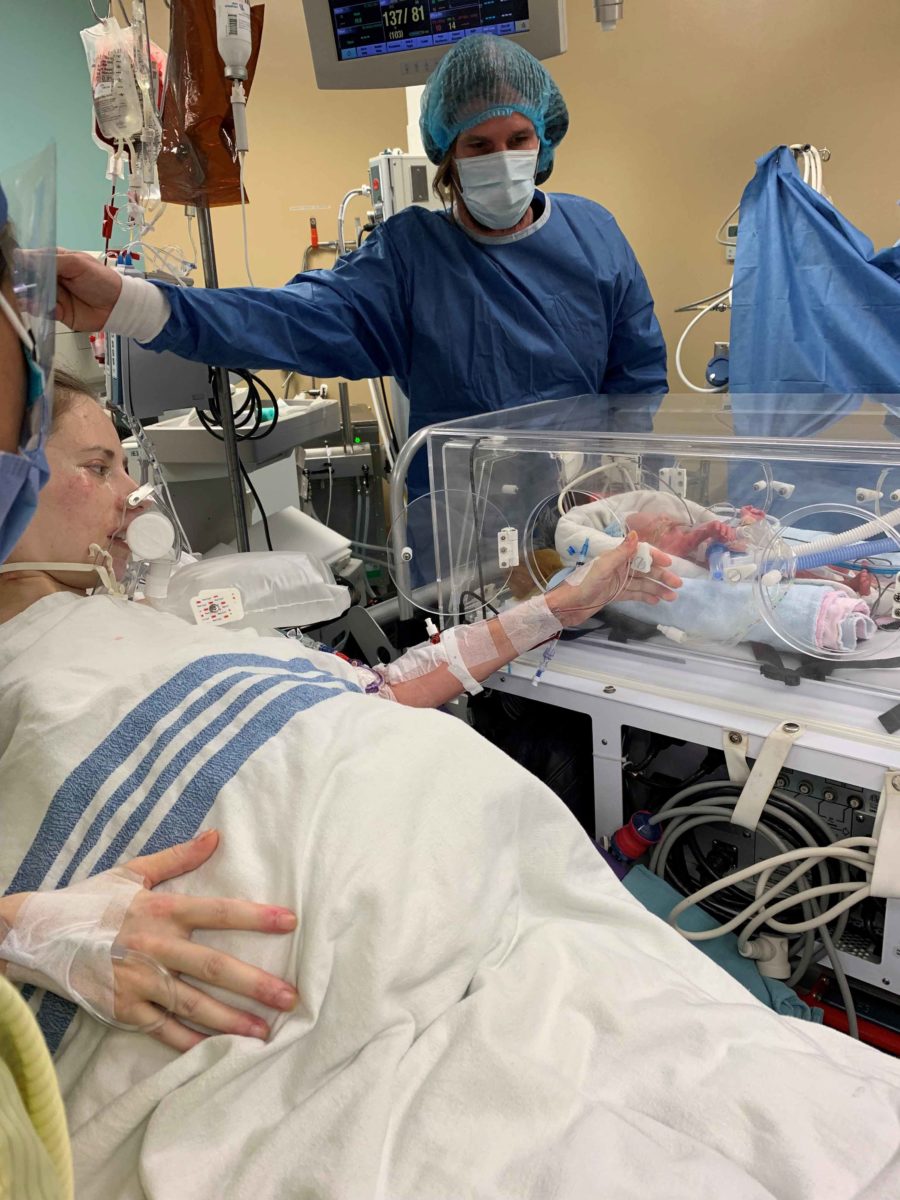
While the other teams were caring for Candice, SickKids’ highly-skilled Acute Care Transport Service (ACTS) team was readying for every possible scenario to support Cameron and transfer him to the neonatal intensive care unit (NICU) at SickKids. The ACTS team typically has access to specialized neonatal equipment through the nursery at the hospital where the delivery takes place, something not readily available to them at Toronto General Hospital. ACTS team members, Jaclyn Murray and Alise Mancini, spent an hour setting up different types of equipment in a separate operating room to ensure they were ready for anything that came up.
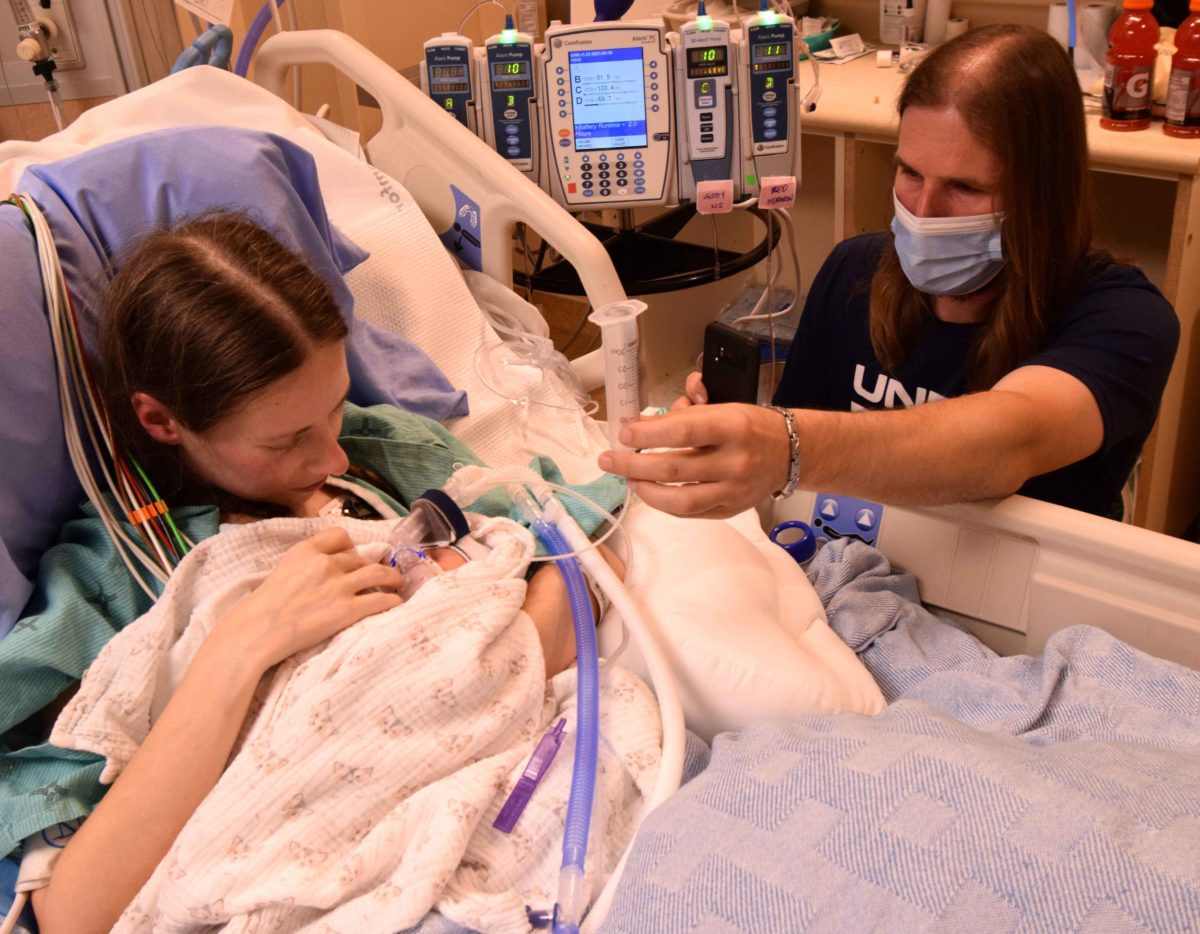
Fortunately, the high-risk delivery went smoothly. After stabilizing baby Cameron, the ACTS team expertly transferred Cameron to the NICU at SickKids for continued care. Eight days later, the ACTS team brought Cameron back to Toronto General Hospital, where his mom remained in the ICU, for a reunion with his parents.
“Preparing for and attending to high-risk deliveries requires an immense amount of pre-planning and teamwork with our adult care colleagues,” says Dr. Estelle Gauda, Head of the Division of Neonatology at SickKids.
The highly skilled SickKids’ ACTS team has exceptional expertise in resuscitating and stabilizing the sickest infants in the province. Once stabilized, Cameron was transferred to the NICU at SickKids where he continued to receive high-level care and thrived. A week later, the ACTS team orchestrated a visit back to Toronto General Hospital so that Cameron could be reunited, if only for a short time, with, Candice and Collin.
“Our motto in the NICU at SickKids is ‘every little thing,’” says Dr. Gauda.
Once Cameron was ready, he was transferred to the NICU at St. Michael’s Hospital until he was discharged home.
Transplant
While preemie baby Cameron was recovering well with the great care of Neonatal specialists at Sick Kids and St. Michael’s Hospital, Candice wasn’t yet out of the woods.
Her condition plus the pregnancy had put a lot of pressure on her heart. Once it became clear that she was not going to improve with medication alone, she was urgently listed for a double-lung transplant. Unfortunately, because of her relative small frame, it was challenging to find a set of lungs that were a match and could fit her chest.
Around a month later, she got her transplant at UHN’s Ajmera Transplant Centre.
The surgery went well, but a few moments after there were a few complications.
“There were complications that can happen with any lung transplant, some inflammation, fluids in her lungs,” explains her thoracic surgeon, Dr. Donahoe.
“It was touch and go for a few days,” she recalls.
For Collin, those hours and days in the surgical waiting room and visiting his unconscious wife in the intensive care unit were the most stressful of this long journey.
“It was the scariest point for me, a constant terrifying feeling that we could lose Candice at any moment.”
With treatment, Candice got better each passing day and her new lungs adjusted to her body. She went home to Midland, Ont., in August and baby Cameron came home shortly after, in early September.
It takes a village
Candice stayed at Toronto General Hospital’s Intensive Care unit for over four months. She and her husband Collin say they only got through such a long difficult journey because of the support from friends, family, and especially from members of TeamUHN, Sinai, SickKids and St. Michael’s.
“I am just so grateful to all the doctors, nurses, physiotherapists, the whole team. They really were like a second family to me,” says Candice.
“I’ll never forget any of them.”
Denise Morris, nurse manager at the Intensive Care unit, remembers how the whole team got invested in this case. And how impactful it was, at a time that COVID had taken a big toll on healthcare workers.
“This case really touched our team. It happened in part during the third wave of the pandemic, when we were losing many young people to COVID. Seeing Candice and her baby have a positive outcome, against all odds, brought joy and a glimmer of hope to everyone involved in their care,” she says.
While Candice was battling for her life and of her child, Collin was also coordinating the family finances and caring for their first child Caitlyn – who turned 13 a few days after her mother’s lung transplant.
“It was a very stressful time for all of our family,” he recalls.
Collin and Candice fondly remember physiotherapist Nathalie Cote and her daily efforts to keep Candice in top shape to receive her transplant. They remember nurse Stephanie Bedford who took the time to knit clothes and a hat for the baby, nurse Sharon Cudek for always taking the time to chat and see how they were doing; nurse Andrea Francis who worked several nights in a row and kept taking extra night shifts to look after them, and so many others. “The whole team was amazing. They didn’t work only to keep Candice and Cameron alive, they really cared,” says Collin.


