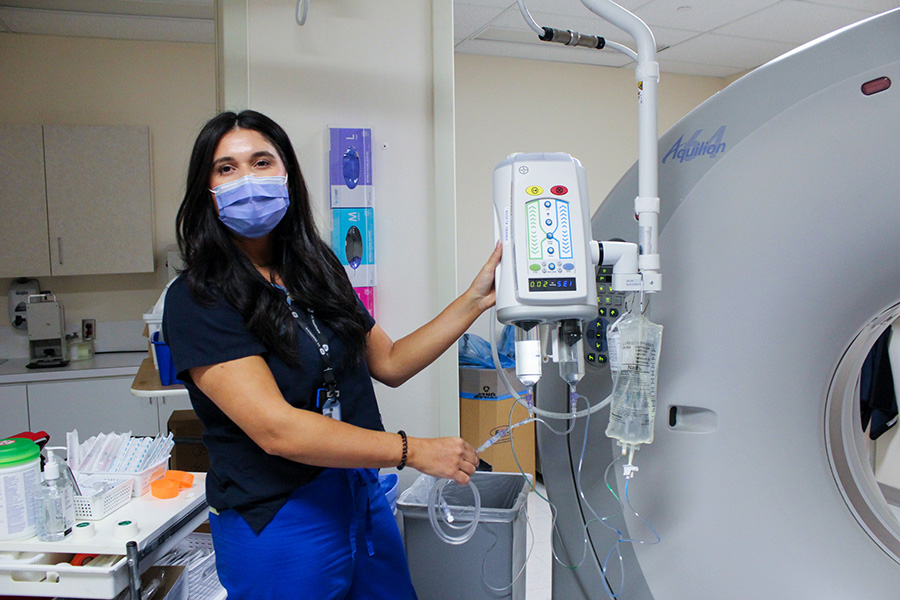
When a patient with a suspected stroke arrives to Toronto Western Hospital’s Emergency Department, seconds can make the difference between life and death.
Paramedics move quickly to transfer the patient onto the CT scanner table where Samantha Mercieca, a medical radiation technologist (MRT), is prepared to efficiently capture 3D brain images with composure and speed.
“These are high-stress situations,” Samantha says. “The team is inside the scan room looking at images in real-time so they can decide if the patient needs to go straight to the Interventional Radiology (IR) suite.”
If the patient is rushed to an IR suite, they are met by a team of professionals including specially trained medical radiation technologists. These MRTs are working alongside vascular surgeons and nurses to provide image-guided procedures such as inserting a stent to control the brain bleed and prevent what could have been a fatal emergency.
November 5 to 11 is Medical Radiation Technologists Week – an annual celebration that recognizes the critical role imaging technologists, sonographers and radiation therapists play in the health care system.
MRTs can work in general X-ray, computed tomography (CT), magnetic resonance imaging (MRI), breast imaging, nuclear medicine, interventional radiology, diagnostic medical sonography, and radiation therapy.
Imaging technologists at the Joint Department of Medical Imaging (UHN, Sinai Health, Women’s College Hospital) performed nearly one million medical imaging procedures in 2022.
In 2018, Samantha graduated from the Joint Medical Radiation Sciences Program offered by the University of Toronto and the Michener Institute of Education at UHN, alongside her classmate Jessica Hughes. Now, they are colleagues at UHN.
Jessica works as an X-Ray technologist primarily at Toronto General Hospital.
“What I like most is that we get to go all over the hospital,” Jessica says. “Every day is different, whether it’s working in outpatient care, emergency X-ray, the operating room, or portable imaging on the floors. It’s fast-paced, and that’s what keeps things interesting.”
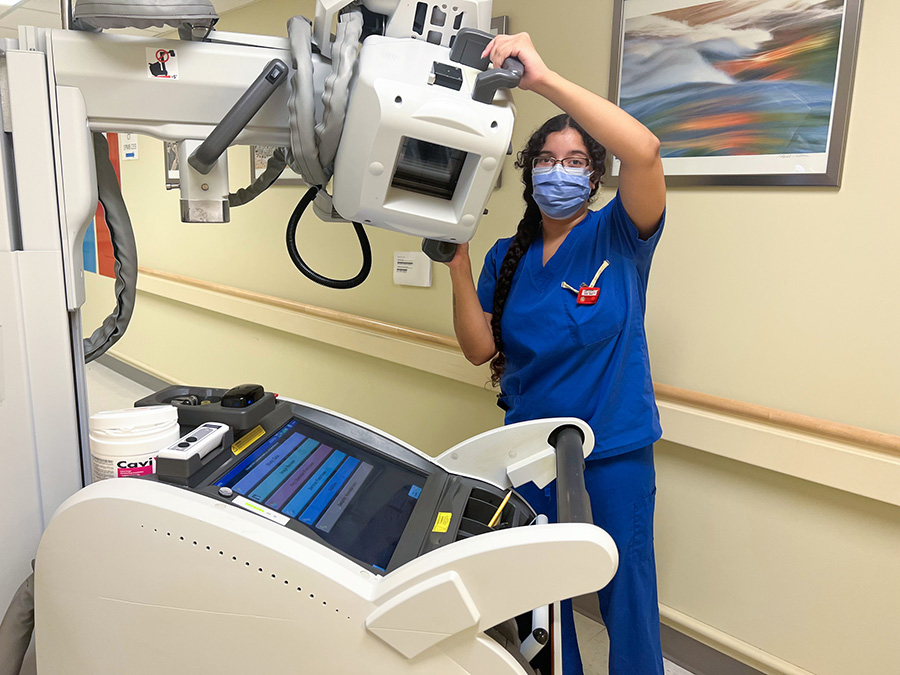
X-rays are an important diagnostic tool that can be critical in several situations from fractures and dislocations to pneumonia, and spinal injuries.
But it’s not just the technology and the diversity of their work that make this profession extraordinary. Jessica reflects on the unique bond they forge with patients.
“At Toronto General, we see a lot of transplant patients,” Jessica says. “We follow their journeys from doing their pre-op images to ICU X-rays and months later as outpatients.
“They remember us, and their names stick in our heads. It’s heartwarming to be part of their transformative journey.”
Over at Princess Margaret Cancer Centre, MRTs play a critical role in cancer diagnosis, staging and treatment. The type of imaging studies conducted depends on the type of cancer, extent and location. For example, an MRI can be used to produce detailed images of soft tissues of the brain or spinal cord, an ultrasound can help identify a pelvic mass, and mammography can detect breast cancer.
Samantha says she frequently performs CT staging scans.
“When they detect cancer, it’s crucial for us to do a staging scan to check for potential spread,” Samantha says. “So, these patients typically come in every three or six months for a full-body scan, so we can monitor and make sure the cancer hasn’t progressed.”
Samantha’s unwavering empathy and compassion are especially evident when caring for patients in these difficult circumstances.
“Many of our patients are quite anxious,” she says. “We do our best to reassure them, thoroughly explain the intricacies of the scan, and help them prepare for sensations like an unusual taste or a warm feeling following the administration of contrast through an IV.”
Down the hall, radiation therapists offer the same level of compassion and dedication as they administer radiation therapy to individuals battling cancer. The Princess Margaret Radiation Medicine Program comprises 180 radiation therapists and is the largest program of its kind in North America.
In 2022, these MRTs provided high-quality radiation therapy treatments to more than 8,000 cancer patients. They are a human bridge between innovative technology and effective therapy during an emotional time in the lives of patients and their families.


