A chance meeting
In February 2009, Rita Spiteri boarded a plane home from Los Angeles to Toronto. But as others opened their books and plugged in their headphones, something compelled her to strike up a conversation with the man beside her.
It turned out her seatmate was a cardiologist returning from a conference where he had spoken on cardiomyopathy – a disease that weakens the heart muscle and can lead to heart failure. Rita could not believe it. Just a couple years ago, she had experienced symptoms that led her family doctor to suspect the very same condition. Yet, despite testing, no clear diagnosis was made.
After hearing Rita’s story, the cardiologist urged her to see a colleague of his at University Health Network’s (UHN’s) Peter Munk Cardiac Centre.
This would save her life.
One diagnosis — a family’s shared reality

Once she landed, Rita called to book an appointment. She was told to come to the Peter Munk Cardiac Centre right away, where she was sent home with a Holter monitor to track her heart rhythm.
Days later while gardening, she felt a sudden wave of weakness and heavy palpitations. Her monitor transmitted the data. The hospital called instantly. Rita’s heart was stopping.
Back in the hospital, an MRI finally revealed the answer to her symptoms: Rita had Arrhythmogenic Right Ventricular Cardiomyopathy (ARVC) – a rare heart condition in which the muscle of the right ventricle is replaced by fatty and fibrous tissue, increasing the risk of irregular arrhythmias and sudden cardiac death.
She was just 47 years old. This discovery would not only impact Rita; it would impact her entire family.
ARVC is a genetically inherited condition. If a parent carries a pathogenic mutation linked to ARVC, each child has a 50% chance of inheriting it. Genetic testing revealed that two of Rita’s three siblings, two of her three children, and one of her brother’s children were at risk of the same fate.
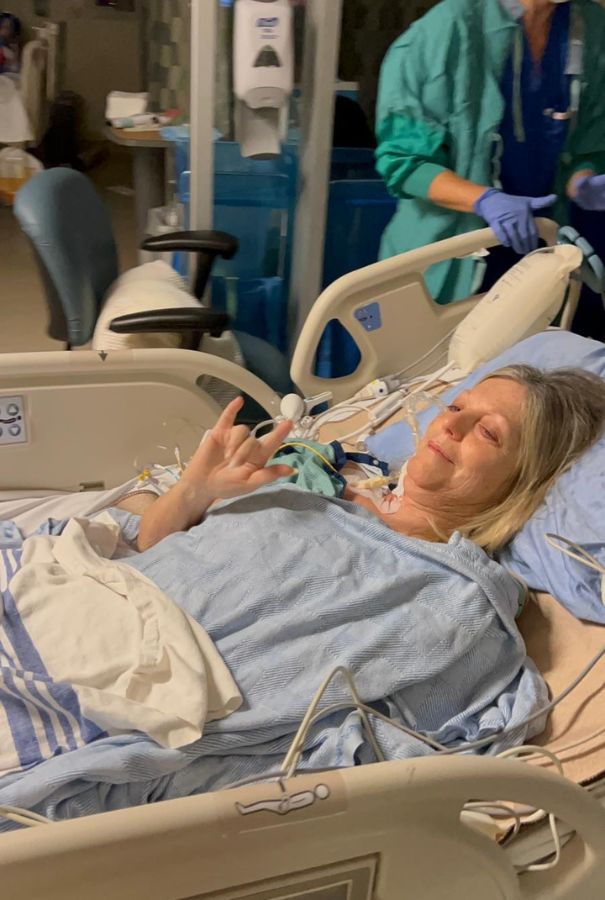
As her family dealt with the news, Rita faced the next step in her own treatment. She required an implantable cardioverter-defibrillator (ICD) – a small, battery-powered device implanted in the chest to continuously monitor the heart’s rhythm. When a dangerous rhythm is detected, the device delivers a high-energy shock to restore a normal heartbeat.
As Rita recovered from her ICD surgery, her sister went into sudden cardiac arrest revealing she needed an ICD of her own. Soon after, her brother was diagnosed with ARVC and was told he, too, required an ICD to support his heart. It wasn’t long before the three of them were being treated together at the Peter Munk Cardiac Centre.
Care at the forefront of discovery
Housed in Toronto General Hospital, the Peter Munk Cardiac Centre is home to Canada’s largest heart failure program and one of North America’s leading inherited arrhythmia programs.
“ARVC is a potentially deadly disease that remains significantly under‑researched,” says Dr. Danna Spears, cardiologist, UHN. “Too often, patients are diagnosed only after a life‑threatening event.”
To address this gap, researchers at the Peter Munk Cardiac Centre are working to better understand the causes of inherited cardiomyopathy and arrhythmia. In 2012, Dr. Spears helped establish the UHN Inherited Arrhythmia and Cardiomyopathy Program — the first in Canada dedicated to the comprehensive evaluation of families with diagnosed or suspected heritable arrhythmias or cardiomyopathies. Today, the Program sees more than 600 patients each year, using genetic testing and advanced imaging to identify biomarkers and more accurately predict risk in individuals and families.
Central to this work is the Peter Munk Cardiac Centre biobank, which houses patient data, tissue and blood samples. Fueled with artificial intelligence (AI) and machine learning, the biobank is accelerating the development of new treatments. It recently played a key role in identifying a biomarker linked to ARVC – a discovery that may clarify how the disease develops, improve diagnosis and, once validated, offer a potential path to stopping its progression.
“By uncovering the genetic causes of cardiomyopathy and congenital heart disease, we are giving patients and families earlier answers, clearer risk and a path to lifesaving care,” says Dr. Spears.
Advancing heart transplant options for patients with inherited heart disease
Unfortunately for Rita, her own diagnosis came too late. By the time her condition was identified, significant and irreversible damage had already been done to her heart – damage that earlier detection might have prevented. In September 2021, she was told she needed a heart transplant.
Two months later, Rita received a call that a heart was available. She was prepped for surgery, but in the final assessment the heart was deemed not viable. She returned to the waitlist – an emotionally difficult but common reality for transplant patients.
“As soon as there is a possibility that an organ may become available, the transplant team acts quickly to prepare the recipient,” says Dr. Seyed Alireza Rabi, cardiac surgeon, Peter Munk Cardiac Centre and lead of the heart transplant program at the Ajmera Transplant Centre. “At the same time, it is essential to honour the donor and their family’s wishes and to maintain a clear separation between their care and the transplantation process. In Canada, these functions are handled by independent teams to ensure trust and transparency in the system.”
To increase the number of hearts available for patients like Rita, UHN is pursuing new approaches in transplantation, including Canada’s first donation‑after‑circulatory‑criteria (DCC) heart transplant in 2025. Led by Dr. Rabi, a multidisciplinary team from the Peter Munk Cardiac Centre and Ajmera Transplant Centre, successfully transplanted a heart which had stopped beating before donation. This milestone is expected to increase the donor pool by 30 per cent.
With 190 Canadians still waiting for a heart in late 2024, these innovations cannot come soon enough.
A new heart – a new purpose

Nearly a year after being listed, Rita finally received her new heart in fall 2022.
She now lives free from ARVC, supported by regular monitoring, a reality she once believed she would never experience. But even as her transplant offers her a new beginning, ARVC remains a heavy presence in her family’s life.
In March 2023, Rita’s 33‑year‑old son went into cardiac arrest during a hockey game. His friends performed CPR on the ice. When the paramedics arrived, they administered five electrical shocks to his heart. It took an hour for them to revive him. Two days later, Rita’s sister died from the same heart disease.
Giving back
Today, Rita has made it her mission to move forward with gratitude and purpose. She volunteers with HeartLinks, a support group for transplant patients at Toronto General Hospital and serves on a national patient advocacy committee working to strengthen Canada’s organ donation and transplantation system. She shares her story widely to encourage others to register as donors.
“My beautiful young heart has given me a second chance at life,” she says. “How could I not give back? If even one person hears my story and becomes an organ donor, I’ve done my job.”
This May, Rita will walk for the second time in We Walk UHNITED, a celebration of unity, gratitude and hope.
“I am overwhelmed with appreciation for every piece of the puzzle that came together and allowed this to happen: the donor and their family, the doctors, nurses and my incredible circle of support at the Peter Munk Cardiac Centre,” says Rita. “But above all, it was my family’s and friends’ unwavering love and strength that carried me to this moment. They stood by me through every step of this journey and I am here today because of them. It is their strength that inspires me to volunteer in the hospital that helped give me the beautiful life miracles I’ve witnessed.”
Rita met a cardiologist on a plane by chance. But her life, and those living with ARVC shouldn’t depend on chance. It depends on a community of donors, researchers and supporters coming together, so more people like Rita can live the full lives they deserve.

No one ever changed the world on their own but when the bright minds at UHN work together with donors we can redefine the world of health care together.