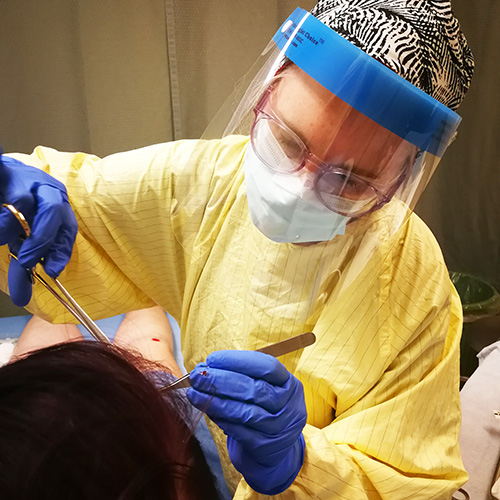
Dr. Erin O’Connor is an Emergency physician at Toronto Western Hospital. (Photo: Talia Ricci, CBC).
Dr. Erin O’Connor has already put in a full day’s work when she arrives at the Toronto Western Hospital (TWH) Emergency Department (ED) for her 4 p.m. shift.
On this day, there were virtual committee meetings, and the planning and administrative duties that come with also being the ED Deputy Medical Director. Plus, there was sharing oversight of her five-year-old’s online schooling with her husband, while the nanny helped with the couple’s three-year-old and meals.
Now, and until early the next morning, Dr. O’Connor’s focus is broken hips, overdose, breaking the news to a patient they have cancer, and COVID-19. Always COVID-19.
“One day last week, of the 19 patients that were here, nine were COVID positive and the other 10 were pending their tests,” she explains. “Almost everyone had something that could have been a symptom.
“We’re really feeling the pressure on the system more in the third wave than we did in the first or second. I think we knew it was coming. I don’t think we knew it was going to be quite this bad.”
By 6:15 p.m., Dr. O’Connor has examined five patients, performed a bedside ultrasound to rule out internal bleeding with one patient, and ordered a multitude of diagnostics. There’s bloodwork. Herpes swab. CT scans of neck, head, and shoulder. Hip X-rays. And in addition, all patients get two automatic COVID tests upon entry to the ED. One rapid, one NP – nasopharyngeal.
Dr. O’Connor suspects two elderly patients have broken hips. One after a fall at home, the other after being hit by a car. The results will take up to a few hours. With families restricted from access during COVID, she phones both patient’s families to inform them of the status of their loved one, and promises to call back once a diagnosis is confirmed. Then, it’s on to the next new admission.
Dr. O’Connor is thankful this third wave has finally plateaued and weekly case counts are slowly declining. But she knows the impact on the hospital system will be felt for a long time by patients.
“Patient care has been stretched, surgeries and procedures have been delayed, and at what cost to morbidity and mortality for patients?” observes Dr. O’Connor.
And then there is the cost to healthcare workers.
“What we see is a system that was strained before the pandemic, that had no stretch capacity and has somehow found the stretch capacity, but really at the cost of those of us working in care,” she says. “Where that stretch has come from is ourpersonal and physical wellness, our resilience, that stretch has come from us.
“What’s stretched in the system is the human factor – those of us who work, and those we serve.”
Dr. O’Connor pauses, choosing her words, then adding for emphasis.
“We’re like ‘okay, it’s a crisis and we’ll use all of our reserves’… there’s been no relief, it’s been constant… there’s no more stretch, there’s no more left.”
Back on the ED, Dr. O’Connor is examining a patient in his early 40s. He arrived by ambulance with decreased consciousness. A suspected opioid overdose. He’s been given Narcan to reverse the overdose. He now seems alert, and asks for a sandwich. Good signs.
Dr. O’Connor’s plan is to try and hold onto him for at least four hours to ensure the Narcan has done it’s work.

Next up, another elderly patient who has fallen, discovered on the floor of her room at a care home. Suspicion is she fell out of bed. The patient has dementia. She utters sounds and yells, but there are no words. After the ritual of donning personal protective equipment, Dr. O’Connor enters the patient’s space, pulling a thick and faded heavy cotton blue patterned curtain closed for privacy.
From the other side of the exam room, a cheery greeting from Dr. O’Connor is heard: “My dear, your nails are so lovely!”
It is a striking moment of humanity amidst the unrelenting strain of this pandemic. Borne of an innate desire to care for her patients and their well-being. A quality Dr. O’Connor is vigilant – and concerned – about retaining.
“Sometimes I wonder if my fuse is a bit shorter or I’m less patient,” she says. “And you worry about ‘compassion-fatigue.’ It’s well documented and well researched as part of burnout that you kind of lose that ability to feel – partially because you’re shielding yourself against it, and partially just because you have no capacity.”
Amongst her colleagues, Dr. O’Connor sees clear signs of burnout. Short fuses. Easily triggered about things that they wouldn’t have reacted to in the past.
“Some are reaching out for help,” says Dr. O’Connor. “Some, I think, don’t really recognize in themselves what is actually happening. For some people, depending on our relationship, I will ask what can be done to help and if they need anything.”
She’s seen a few already leave the profession. Others have confided to her they will retire once the pandemic ends. There is no desire to go through this again.
Just after 8 p.m., diagnostics start coming back. The patient with the lovely nails has a slight fracture in one shoulder. The best course of action to healing is keep the shoulder immobile and put the arm in a sling.
Unfortunately, both of the suspected broken hips are confirmed. Dr. O’Connor knows a fractured hip is associated with an increased mortality rate in the elderly. Both require emergency surgery. Dr. O’Connor pages the orthopedic resident to come assess the patients for surgery, and starts the process for both to be admitted. Then, there’s the calls to the families.
At 8:40 p.m., Dr. O’Connor sees a small window of opportunity for dinner. She lets her colleagues know, then heads down a long corridor to the TWH ED change room. It is quiet here, away from the constant cacophony of intercom pages and announcements, capsules being sucked up the pneumatic tube system, and ringing phones. Although, it’s certainly not what you’d call a sanctuary.
The room is cramped. There are rows of lockers lining the walls around the room. On top of the lockers, sit knapsacks and shoes. On the floor, around the edge of the room, are more knapsacks and shoes. In the middle of the room is a small two-seater couch and low-rise table laden with alcohol wipes, hand sanitizer, and a box of granola bars brought in by a colleague. To one side, there’s a small table with a computer, and most curious, in a corner to the left of the computer stands an old portable folding three-panel wooden screen divider. Behind this screen, is the privacy afforded every ED doctor of all sexes to change in and out of scrubs.
Who says ED life is glamorous.
Dr. O’Connor chats with a few colleagues as she nibbles on dinner – a cheese stick, pepperoni stick, and water. All three people try to stay physically distanced in this claustrophobic space. Dinner complete, Dr. O’Connor continues the conversation while reaching into her pocket. Out come a few small pieces of her five-year-old’s LEGO. She rolls them in her fingers and smiles. Then, she just holds them. They appear to bring a small measure of comfort.

After the 15-minute dinner break, Dr. O’Connor is back in the middle of the ED. Sitting at a computer amidst the bustle and sound of the Acute/Sub Acute Nursing Station. She’s running down the status of each of her patients. Reading diagnostic assessments.
She is asked how she is doing.
“I mean, certainly there’s definitely fatigue, and it ebbs and flows right? And it depends on the day…and what’s happened,” explains Dr. O’Connor. She stops. Her eyes are tearing. Clearly, it has been one of those days where something happened. She composes herself.
“Sorry, that’s going to happen…but it’s actually not that bad.”
Another pause, more composing.
“One of the things that’s been really helpful is colleagues. There are a few of the people in the department who are friends you can call at any time and just talk it out. To know someone else is feeling that burden, it’s a huge difference. And then, trying to carve out time where you get a little more sleep. And, try as much as possible when I can to really just focus on kids and family.”

A nurse arrives to tell Dr. O’Connor the overdose patient wants to leave. It’s been close to four hours. She hustles over for one last examination to ensure it is safe for him to be discharged.
Another patient arrives. Another elderly woman has fallen. The diagnostics will come back all clear. Thankfully, all that’s required is a few stitches over one eye.
For all the strain of the pandemic, Dr. O’Connor is quick to point out there are positives that will have a lasting benefit to patients.
“Virtual models of care will benefit patients with disabilities and elderly patients in the future,” she says. “Not needing to leave their homes for follow-up or simple medical appointments hopefully will allow for more equitable access to care.
“And, maybe, just maybe, the pandemic will be the start in a shift back toward trust in expert opinion. There has been a movement in popular culture in the past few years away from trust in experts and education, maybe this will help people to change their minds. Though the anti-maskers and anti-vaxxers are still loud!”
By 12:30 a.m., Dr. O’Connor is delivering a brief handover to her colleague in charge of the overnight shift. Of all the patients in her care this past evening, the majority have been discharged or been admitted. There’s just the lady with the stitches awaiting her discharge paper work. And one of the broken hip patients is awaiting orthopedics admission.
“At the end of the day, I love my job,” she says. “I’m so lucky that I get to do this…
“I have the best job in the world and I love where I work and I love the people I work with.
“I’ve been so very privileged to be able to be their leader and have their faith and their confidence.
“And, I am so immensely privileged that I get to do this job.”


