While the PE can be treated by blood thinners, the CTEPH must be treated through a very long and complicated pulmonary thromboendarterectomy (PEA) surgery. There is a steep learning curve for thoracic surgeons to learn the procedure that has a high risk of mortality. Currently, PEA is only offered at a few specialized centres in the world.
Patrick Himmelheber is grateful Toronto Western Hospital is one of these centres.
When Patrick couldn’t catch his breath during his first recreational hockey game of the season in the fall of 2015, he just thought he had let himself get out of shape over the summer.
“It was the beginning of the season and I got winded as soon as I got on the ice,” recalls Patrick. “I figured I really needed to work on my cardio, but it got to the point that I couldn’t play without getting short of breath and I quit the team.
“It was very weird to be so short of breath because I’m a pretty fit person and exercised regularly,” he continues. “But every time I exerted myself, even to go up the stairs, I couldn’t breathe.”
Patrick struggled with his condition for eight months and finally decided to broach the issue with his doctor at Toronto Western Hospital’s Family Health Team. Since he otherwise felt fine and really wanted to underscore the degree to which he was short of breath, he asked Dr. Taylor Ferrier if he could demonstrate by walking up a set of stairs together.
As they walked up the stairs, Patrick’s breathing immediately became laboured, he couldn’t talk and had to stop to catch his breath.
Dr. Ferrier suspected PE and first ordered blood work but it came back showing nothing out of the ordinary. He spoke to his peers and the consensus was to do a CT scan to be safe. The scan revealed that Patrick had blood clots in both of his lungs. He was immediately sent to the Emergency Department, put on blood thinners and admitted overnight for observation.
“Later on, my family doctor would tell me that I was lucky to be alive,” says Patrick. “The amount of clotting they found in my lungs would have been detrimental to anyone who hadn’t been as physically active as I was.”
Patrick would need PEA surgery
Once stabilized, patients who experience PE are referred to Toronto General Hospital’s CTEPH Clinic for follow-up. Patrick went for his appointment a few days later where he was prescribed a twice daily injected blood thinner for a month and scheduled for further follow-up in the fall.
Patrick went on with his life; travelling, enjoying the summer and spending time with his wife. As his follow-up appointment day approached, he figured it would be a routine formality. But the day before, Patrick’s morning routine was interrupted by sharp pain in his chest.
His wife rushed him to the Emergency Department where he was relieved to hear that he didn’t have any new clots. However, the diagnosis was very concerning: as a result of his earlier PE, necrosis – a side effect of CTEPH – was taking hold of his right lung and a very small part of his lung had died from the lack of blood flow in its arteries.
The chest pain was a result of the scar tissue from the necrosis pushing on his chest, and he would need surgery to remove it. Individuals with CTEPH that is left untreated can die within three to five years.
After a summer of feeling relatively secure about his diagnosis and treatment, Patrick now found himself seated across from a thoracic surgeon with an uncertain future ahead.
Fortunately, the thoracic surgeon in question was Dr. Marc de Perrot,Surgical Director, Pulmonary Hypertension/CTEPH Program, UHN, whose expertise focuses on procedures for end-stage lung diseases including CTEPH, which is treated via PEA.
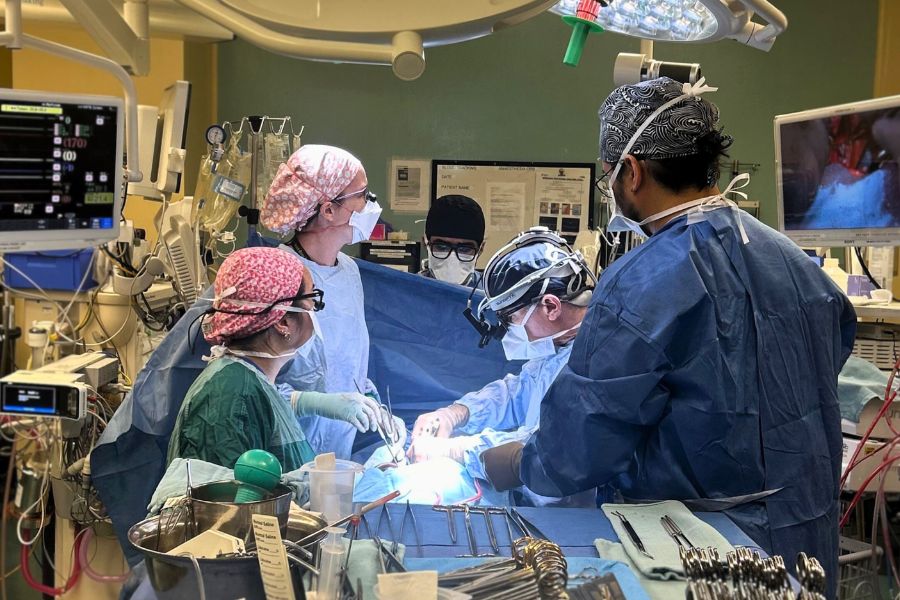
PEA is one of the most challenging procedures to teach and learn in cardiothoracic surgery.Working in a lung’s artery with magnifying glasses is delicate work making the technique difficult to teach – only one surgeon at a time can look through the artery during the procedure to see all the intricate detail.
Less than a month after his consultation with Dr. de Perrot, Patrick underwent an eight-hour surgery to separate and remove the scar tissue from his lungs’ arteries.
For Patrick, it was happenstance that connected him with Dr. de Perrot – as an existing patient at UHN, he was referred to the appropriate physician who had the specialized expertise and skill to diagnose and treat his condition.
But there is a steep learning curve for thoracic surgeons to learn the PEA procedure that can result in high risk of mortality.
“Thoracic surgeons learn PEA by assisting during the procedure,” explains Dr. de Perrot. “Working in a lung’s artery with magnifying glasses is delicate work making the technique difficult to teach – only one surgeon at a time can look through the artery during the procedure to see all the intricate detail.”
As such, learning the procedure can take about two years, making it difficult to more quickly enlarge the pool of surgeons who can offer PEA. Thanks to donor support, Dr. de Perrothas spent a year developing a visual simulator, which aims to reduce training time for the procedure by six months – helping more people survive than ever before.
Following his surgery, Patrick felt an immediate difference. He has returned to normal life and was back to work on the two month anniversary of the procedure. Since then, he and his wife have welcomed a child, and he’s back to working out and enjoying life with his wife and daughter.
Looking back, Patrick realizes just how serious his condition was, and takes nothing for granted. Including the generosity of donors who make care like he received possible.