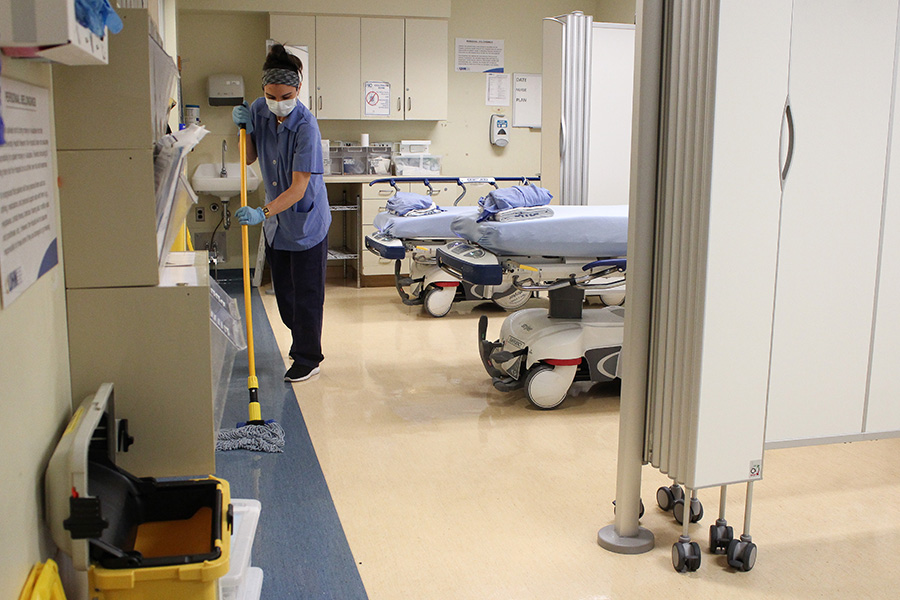
Priscilla Sousa has worked in Environmental Services at UHN for six years. She loves working in the Emergency Department at Toronto General Hospital because it’s fast-paced and the staff are like family. (Photo: UHN)
By 7:15 a.m. – just 15 minutes into her shift – Priscilla Sousa has already cleaned three rooms in the Toronto General Hospital (TGH) Emergency Department (ED).
As an Environmental Services aide – more commonly known as housekeeper – in the ED, time is of the essence, especially during a pandemic.
Priscilla has worked in UHN Environmental Services, part of the Facilities Management – Planning, Redevelopment & Operations (FM-PRO) Department, for six years. She started as part-time casual, working on various floors across TGH, before landing her fulltime shift in the ED, Monday to Friday from 7 a.m. to 3 p.m.
While a thorough clean is important across all units in the hospital, pace is an added factor here.
“We don’t know what it’s going to be like in Emerg, so the more you get done early, the better it is,” says Priscilla. “When a room gets discharged, there’s usually another patient waiting for a room, so the speed has to be a bit faster here.”
On a good day, the mornings are calm, so she can get her daily cleaning done before patients and paramedics start flooding in.
Priscilla is one of three Environmental Services aides working the same shift. The ED is divided among them. Priscilla starts in the Rapid Assessment Zone and works her way towards the centre of the department. Each room in her area, including nursing stations and medical equipment rooms, must be cleaned at least once per shift, on top of thorough cleanings of patient rooms after a discharge, and any unplanned spills and messes.
“I need to come if there’s a mess from casting … or if somebody vomits, urinates, or if there’s feces,” she says. “We get a lot of that.”
She also cleans the washrooms and empties the garbage cans in her section at least three times per day.
As she goes through her allotted rooms, Priscilla cleans everything – literally. She starts with high dusting (ceilings, fans, vents) and works her way down. The walls get wiped with disinfectant, all high-touch surfaces – such bed railings, call buttons, light switches and door knobs – counters, which are coarse and damaged from the constant bleach, cupboards, handles, equipment, wires and even the outside of the garbage can. Finally, she sweeps, then mops her way out of the room, puts up a wet floor sign and does it all over again next door.
It’s physical work, which has only become more taxing with added COVID-19 protocols.
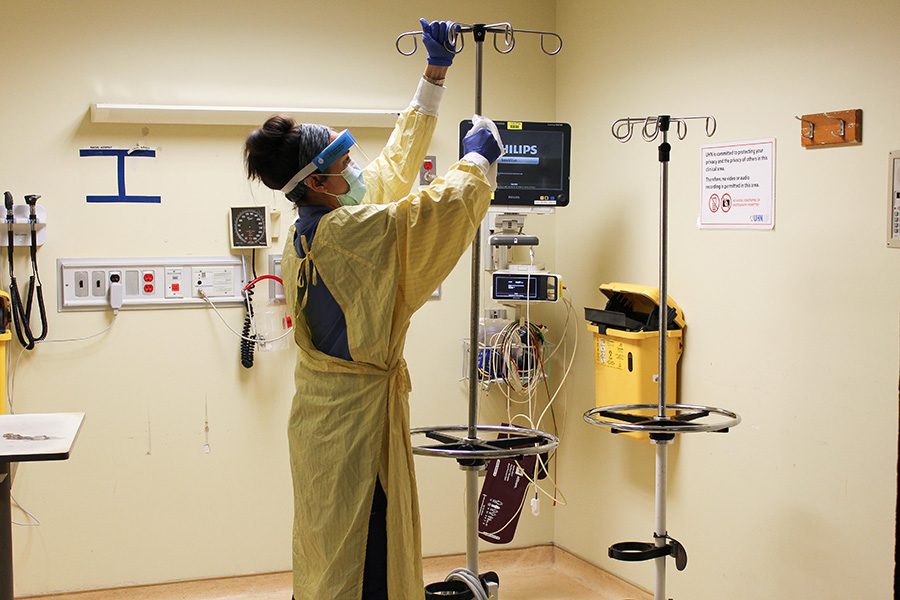
“It’s a lot harder due to wearing a mask constantly now,” she says, adding that she also wears a gown and face shield when cleaning a room after a patient gets discharged, regardless of their COVID-19 status.
Before the pandemic, Priscilla would only don this gear when cleaning an isolation room – now it’s Infection Prevention and Control (IPAC) protocol as an extra precaution.
In the beginning, it was a lot to get used to.
“It was tiring. It was hot. It was new and scary,” says Priscilla.
It’s especially unnerving in the ED, because, in some cases, staff don’t know right away if a patient has COVID-19.
“We have to treat everything as if it’s COVID-positive,” she says. “Everything is running through your head: ‘Did you wipe everything? Did I get it on my pant leg (because our gowns don’t go all the way down)?'”
Now, on this day, in what is hopefully the tail end of Wave Three, “it’s all become normal,” says Priscilla, adding that many of the new IPAC protocols will likely remain moving forward. For example, all supplies – such as gloves and paper towels – are kept outside of patient rooms, to avoid potential contamination.
Curtains were also removed from inside patient rooms and bolted to the wall on the outside, so they don’t have to be taken down and washed after every patient, unless the person is COVID-19 positive.
There are also “little things” Priscilla changed about the way she works, like keeping her hair in a bun instead of a ponytail and wearing shoes without laces, which means there’s one less thing to touch.
Her colleague, John Marinelli, also takes precautionary measures at home, to keep his wife and nine-year-old daughter safe.
“When I get home I head straight down to the basement, remove my clothes and shower,” he says. “I don’t even say ‘hi’ to them.
“That still happens today – they know the routine.”
While it’s been a stressful – and exhausting – year-and-a-half, it helps that the ED staff operate like a family. They go in on the lottery together, share life updates and lend a helping hand whenever they can.
“I’ve had patient care assistants and nurses grab my mop and mop something,” says Priscilla. “It’s how it works – we help each other all the time. We’re the dream team.”
ED Manager Debra Davies agrees and gives well-deserved credit to Priscilla and her colleagues.
“Honestly, our Environmental Services team here, they’ve kept us safe during COVID,” says Debra.
“They’ve done all the heavy lifting.”
As Priscilla continues with her daily cleaning, the needs of patients are always top of mind.
She directs a lost patient to the nearest washroom, gives another fresh towels so he can freshen up and, most importantly, listens to them.
As she enters a patient room to bring in a clean table, the patient confides in her that they don’t feel comfortable with a male nurse due to a childhood incident.
“I’ll let somebody know,” Priscilla reassures the patient, before tracking down the medical team to alert them.
Another patient asks for sugar for his cereal.
“Let me check with your nurse if you’re allowed to have it,” she tells him.
Medical staff tell her the patient can’t have sugar due to medical restrictions, so Priscilla passes on the message with care.
“I can’t give them anything without checking,” she says. “We don’t know what tests they could be doing, or what their issues are – even a glass of water or a cup of ice – we check first.”

By noon, her daily cleans are completed, so she checks a digital screen that lists patient rooms, admissions and discharges. There’s nothing outstanding, so she sees if John needs any help.
They chat and joke around for a minute, until a patient gets discharged. The chit-chat stops, they don their gowns and face shields and get to work disinfecting the room.
They strip the bed and wipe down every nook and cranny – the walls, the mattress, beneath the mattress, bed railings, all equipment, wires, screens and high touch surfaces. Once they’re done, they dispose of their PPE and immediately wash their hands.
By the end of this mid-June shift, Priscilla checks the system and confirms only one patient was tested for COVID-19.
It came back negative.
Days like this are becoming more common and ED patient visits are returning to pre-pandemic numbers.
“When cases were high, I think people were more so afraid to come in – the waiting area was empty,” says Priscilla. “With second doses of vaccine rolling out, it’s coming back to normal now.”
While the light at the end of the tunnel appears to be getting brighter, Priscilla’s job – like the rest of her ED family colleagues – is forever changed.
A mask is part of her uniform now and she will always be on high alert. “We can’t let our guard down,” she says. “I’m not nervous anymore, but I don’t want to catch anything either.”


