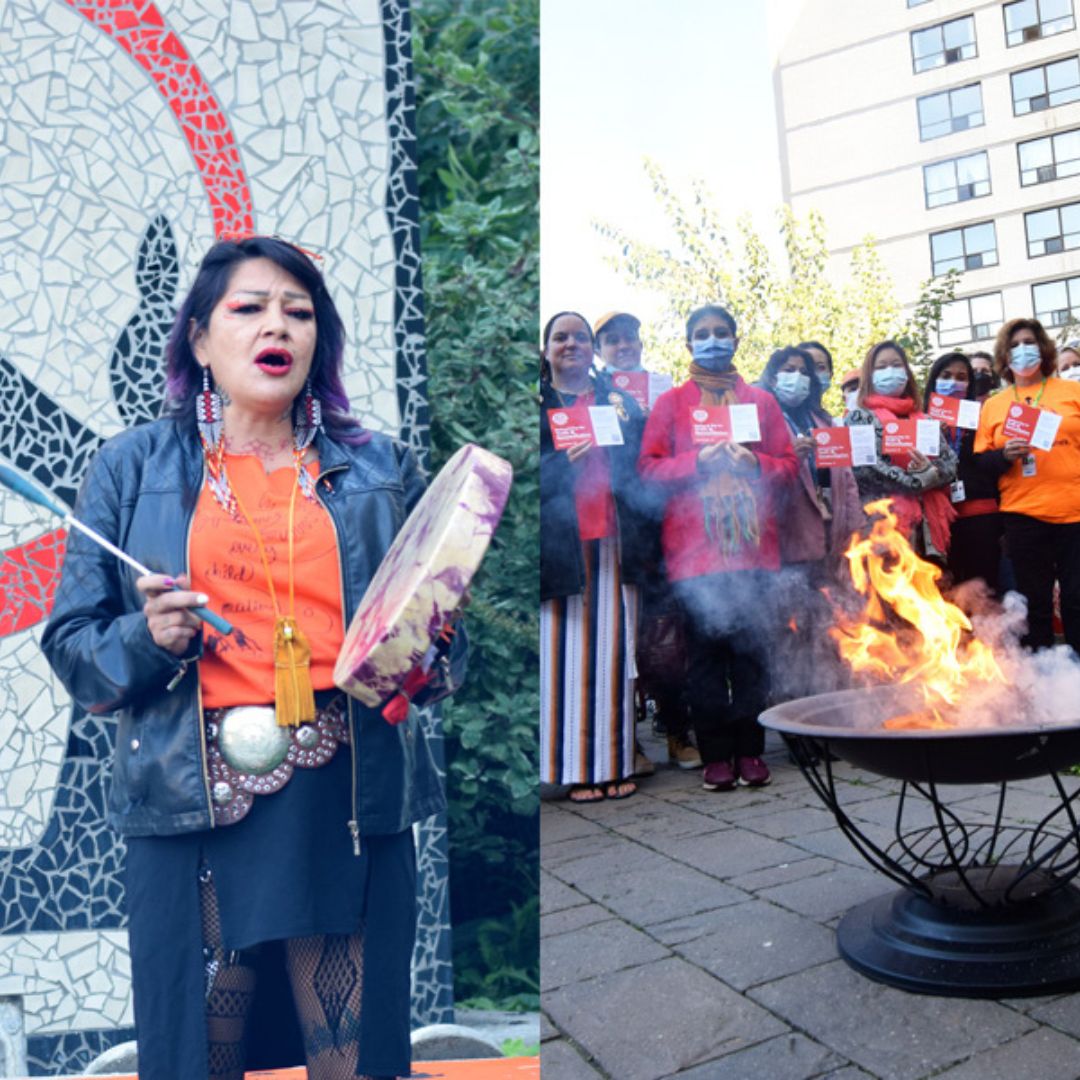Victoria Manitowabi, (L), and Chantell Morais are the two new Indigenous patient navigators in the UHN Emergency Department. The goal of the initiative is to make the ED a safer space for the Indigenous community to access care. (Photo: UHN)
The professional and life experiences of Chantell Morais and Victoria Manitowabi have perfectly positioned them for a new role as Indigenous patient navigators in UHN’s Emergency Department (ED).
Chantell, a Haudenosaunee woman who is Mohawk and Irish, and sits with the Bear Clan, is a longtime Indigenous case manager and harm reduction worker who has vast experience with the negative impact hospitals can have on community members.
“I’ve been in and out of the hospital with so many community members over the years,” says Chantell, who will be based at Toronto Western Hospital. “Sometimes I have wished that the care was different or the support was more culturally appropriate and people were more understanding of some of the traumas, such as intergenerational trauma or personal traumas, associated with colonization.
“I wish the care was more tailored to First Nations, Inuit and Métis people.”
The Indigenous Health Program (IHP) and UHN’s Emergency Medicine team have partnered to introduce the Indigenous Patient Navigators (IPN) in the ED – Chantell at TWH and at TGH is Naaniibwid Genoozid Zhingwaak Kwe, whose given name is Victoria Manitowabi.
The goal of this initiative is to make the EDs a safer space for the Indigenous community to access care.
“Our community has faced a lot of discrimination and racism in health care,” says Victoria, who is Anishinaabe Kwe from Wiikwemkoong Unceded Territory on Manitoulin Island.
“They don’t feel safe coming in to get the proper health care even if they know they need it. There are barriers stopping them.”
TD Bank Group (TD) is supporting UHN’s Emergency Medicine team and Indigenous Health Program (IHP) to improve health equity in the Emergency Department (ED) for First Nations, Inuit and Métis Peoples. The $1.48 million gift from TD will help fund the merging of Indigenous and Western approaches to provide urgent and equitable care across UHN’s two EDs located at Toronto General and Toronto Western hospitals.
The experience of Indigenous peoples with colonial institutions, including the health care system, has been fraught with bias, cultural and systematic oppression, and racism.
Historical and ongoing harm and trauma has resulted in a mistrust of the health care system and delays or avoidance of accessing needed health care, including the ED, where community members are often turned away or misdiagnosed. These perpetuated harms result in negative health outcomes, such as reduced life expectancy and increased rates of chronic disease.

These are some of the reasons that the ED Indigenous patient navigator’s role is so important, and why both Chantell and Victoria are determined to start eliminating some of these things within UHN.
“Many patients visit the ED not just for medical needs, but for social needs as well,” says Dr. Marcella Jones, a staff physician and the Co-Lead for Health Equity in the Emergency Department. “Our partnership with the IHP is key in building trust between us as a health care organization and the Indigenous communities that we serve.”
In addition to the new IPNs in the ED, the IHP will offer cultural methods of care, including use of the four traditional medicines – tobacco, cedar, sage and sweetgrass. IHP team members will also be providing safe spaces for Indigenous patients to access ceremony, as for many Indigenous peoples, it is a daily practice which offers strength, grounding and cleansing of our spirits.
“The Indigenous Health Program is about transformative medicine,” says Leonard Benoit, Indigenous patient navigator for IHP and the Indigenous Cancer Program.
“It’s about bringing the ways of Indigenous people into health care and making sure it’s accessible and equitable so that Indigenous folks can actually have treatment the way they decide, as opposed to it being told to them.”
Ashley Migwans, Operations & Program Manager of the Indigenous Health Program, says, “the IHP and Emergency Medicine teams have come together to break the cycle of negative health and wellness outcomes that currently exist within the health care system, by incorporating Indigenous knowledge, practices, and systems into the existing framework.
“This revolution in care will include guidance and feedback from community, educational resources, and cultural safety training for staff,” Ashley says. “Chantell and Victoria will be pivotal in this journey, not only to patients, but also to staff.”

Under this new initiative, patients who identify as First Nations, Métis, or Inuit that come into the ED can connect with the IPNs for support, either through staff-referral or self-referral.
Digital screens and posters will be displayed in the ED to announce the roles and provide more information for patients, so that they can request the extra support if needed.
The IPNs will also be able to offer support beyond the ED. If someone is transferred to another floor for care, Chantell or Victoria will still be on the care team, offering both culturally appropriate support and connection, and community space allowing them to feel safe.
“Our community has always taken care of each other since the beginning of time,” says Chantell, who completed her bachelor of arts in sociology from York University and her masters in gender studies and feminist research from McMaster University, focusing on the misuse of solitary confinement against Indigenous women in the Canadian prison system.
“We are not individualistic people. We are community, and community cares for community.”
Chantell and Victoria will be able to provide direct one-to-one support to Indigenous patients through provision of information, resources, advocacy and coordination of services; facilitate requests for access to Indigenous ceremonies and medicines; facilitate connections with family, Elders, traditional healers and other community supports, and participate in case discussions and debriefs.
“We always want people to come into our circle, be a part of it, ask questions, see the way we do things, and start building relationships with each other,” says Victoria, who was a prenatal and postnatal case manager at Toronto Birth Centre and went back to school for her social service degree.
“This initiative is a great opportunity to not only bring more health care providers into our space, but others as well.”