It starts with an unimaginably precious gift: another chance to live.
The generosity of organ donors means the world to people whose lives they save. The reality is that not every organ can be used. Damage, disease and incompatibility with the recipient mean that in hospitals around the world, that gift of life is lost.
TeamUHN has found a new way.
Healing organs and saving lives with EVLP
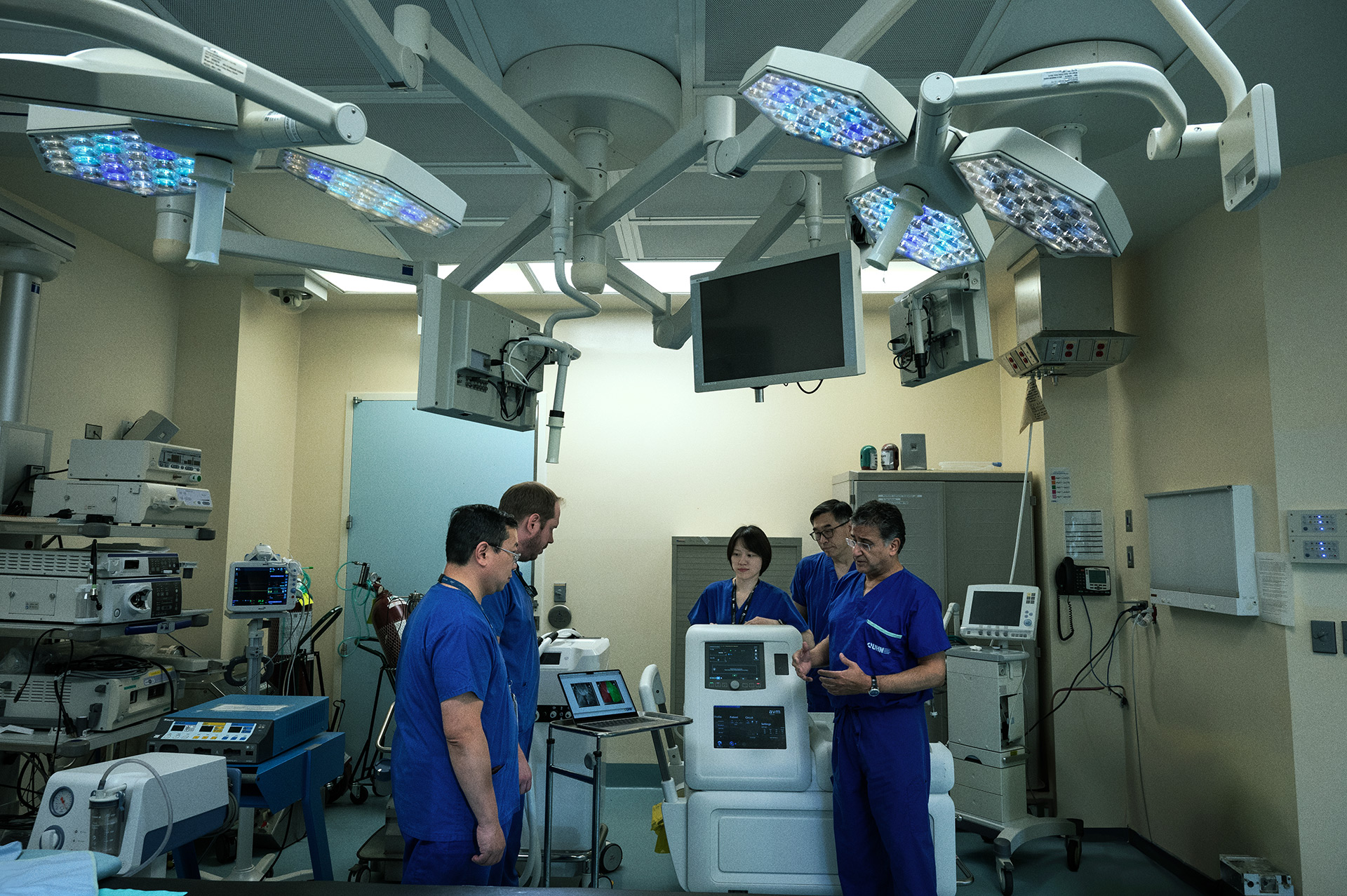
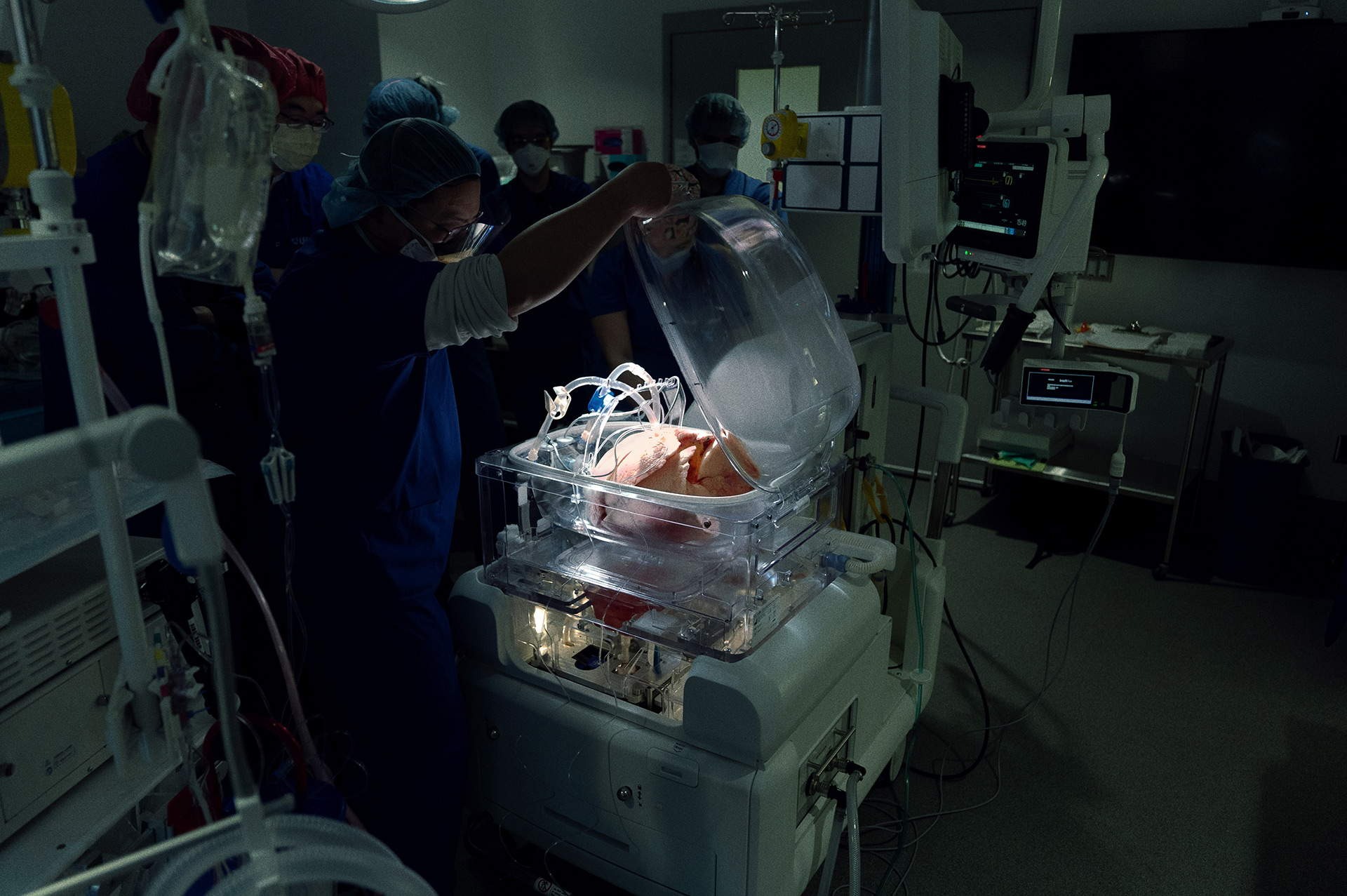
In highly-specialized operating rooms at UHN’s Toronto General Hospital, Manyin Chen and Hongchao Shan, organ perfusion specialists, are making transplantation more successful using UHN’s homegrown technology known as the Toronto Ex Vivo Lung Perfusion (EVLP) System.
It may look like science fiction, but EVLP has been helping TeamUHN increase the number of transplants since 2008.
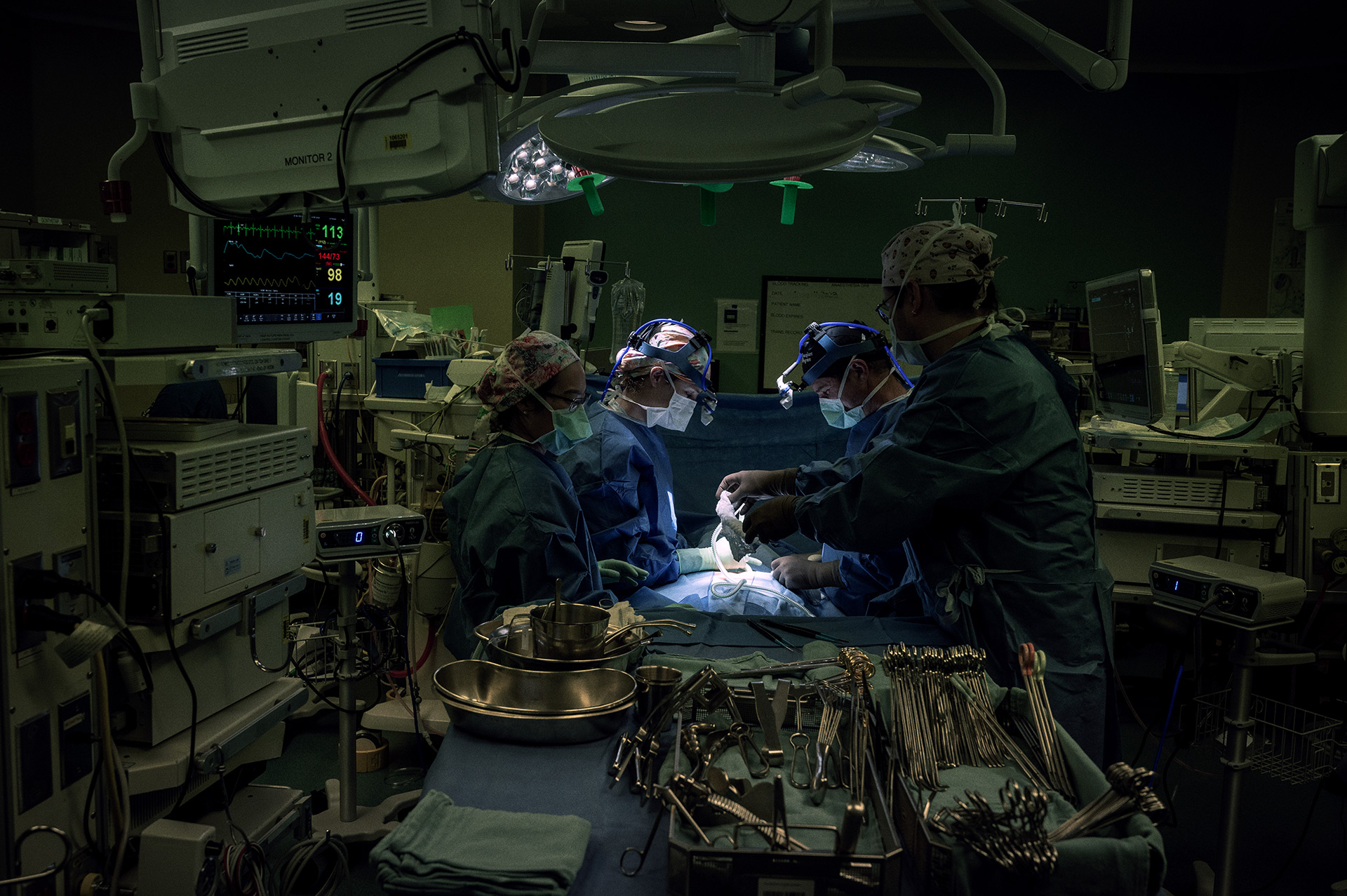
As organ perfusion specialists, Manyin and Hongchao use EVLP to do the delicate work of keeping lungs “alive” and stable outside of a body before transplantation. The surgical team assesses and treats the lungs to ensure they are functioning well and are ready for transplant. Infections that would otherwise make lungs unusable can be treated, meaning surgeons can perform more transplants and save more lives.
With EVLP, UHN’s Ajmera Transplant Centre performs more lung transplants than anywhere in the world.
UHNITED to solve transplant’s biggest challenges
While organ perfusion specialists like Manyin and Hongchao are working with EVLP to support life-saving transplants for patients today, their colleagues’ innovations are changing transplantation for tomorrow.
Trailblazers leading this work are EVLP co-inventors, Dr. Shaf Keshavjee, Director of the Toronto Lung Transplant Program. Director of the Latner Thoracic Surgery Research Laboratories and the Chief of Innovation at UHN and Dr. Marcelo Cypel, Surgical Director of the Ajmera Transplant Centre and Senior Scientist in the Latner Thoracic Surgery Research Laboratories. They are dedicated to developing EVLP’s potential to solve some of the biggest challenges in transplantation.
One of the challenges at the top of the list? Organ compatibility.
Patients can only receive organs that are compatible with their blood type. For patients with rare blood types, this means longer wait times and worsening symptoms until a match becomes available. This can also mean organs go unused because a compatible patient is not found in the short window of time an organ can be preserved for.
EVLP is already making it possible to preserve lungs for longer. Now, Drs. Keshavjee and Cypel and their team have shown that they can use EVLP to treat lungs with a special process that can change the organ’s blood type – a breakthrough that will save more lives and make every transplant a better match for each patient.
Accelerating transplant research with artificial intelligence and machine learning
When inventors like Drs. Keshavjee and Cypel can work alongside artificial intelligence (AI) and machine-learning experts, game-changing innovations like these happen faster. Dr. Andrew Sage, Assistant Scientist, Toronto Lung Transplant Program, Ajmera Transplant Centre, is working with the team to harness the power of AI and machine learning to improve the success of EVLP technology and bring it to more hospitals around the world.
Together, they have developed a tool that will give transplant teams the power to make faster and smarter decisions with machine learning-guided analysis. With data-driven guidance, transplantation will be safer and available to more patients worldwide.
From machine learning experts in the lab to organ perfusion specialists in the operating room, TeamUHN is UHNITED in redefining the future of transplant.

No one ever changed the world on their own but when the bright minds at UHN work together with donors we can redefine the world of health care together.