A UHN study is testing a world-first treatment for lung damage caused by COVID-19
As researchers around the world continue to seek effective treatments for COVID-19, a team at University Health Network (UHN) is exploring a first-of-its-kind therapy that aims to treat respiratory failure using injections of decidual stromal cells (DSC) drawn from human placentas.
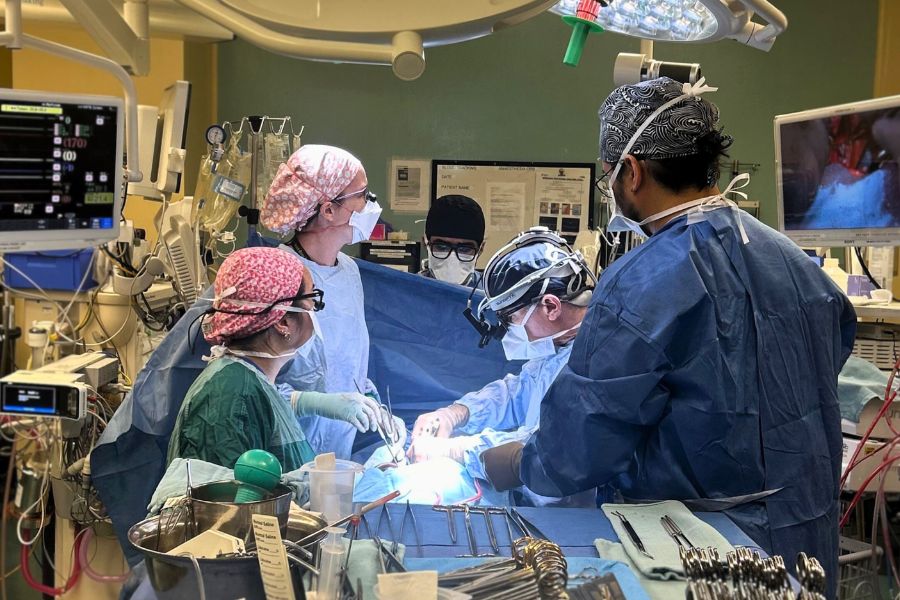
DSCs are natural immunosuppressants that protect the mother and fetus from each other’s immune systems and help ward off infection. They are collected from placentas donated after caesarean section births, and are cultured and grown before being diluted and injected into a patient’s blood stream. The cells then travel to damaged tissue within the lungs where – based on this study’s hypothesis – they inhibit immune response only in the affected area.
Led by Dr. John Granton, Medical Director of Health Services at UHN and Dr. Jonas Mattsson, Director, Hans Messner Allogeneic Transplant Program, Princess Margaret Cancer Centre and Gloria and Seymour Epstein Chair in Cell Therapy and Transplantation, UHN, the study aims to use the immunosuppressive qualities of DSCs to treat COVID-19-related lung injury, which is caused both by the virus itself and by the body’s immune response.
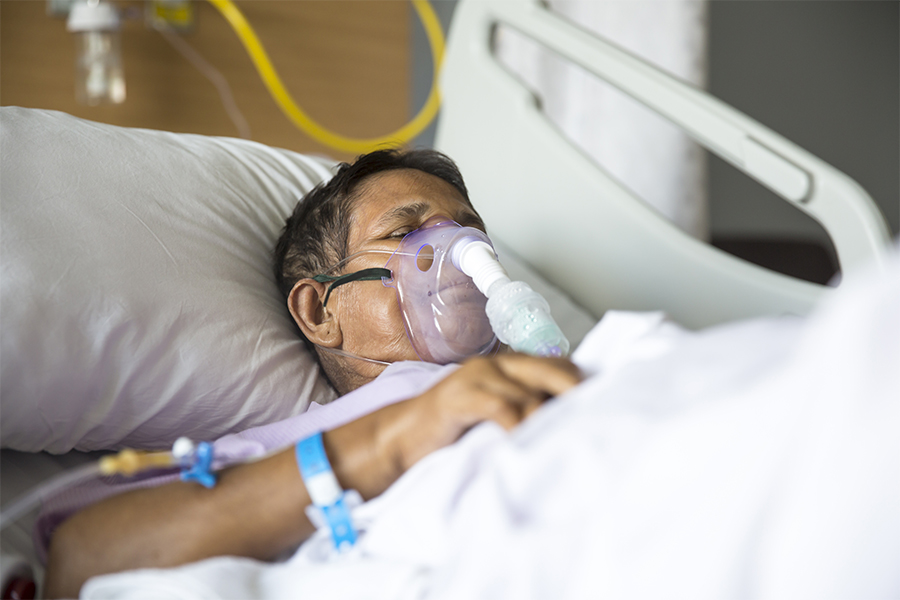
Severe immune responses can cause inflammation and damage to lung tissue. Significant damage leads to respiratory failure, meaning the patient can no longer breathe on their own. The next step for patients is critical care and often the use of a ventilator, but treatment options are limited without an effective therapy to address the lung damage.
Drs. Granton and Mattsson believe that suppressing the immune response with DSCs could help prevent further damage and give the lungs a chance to heal.

Harnessing natural immune properties
Dr. Mattsson was previously involved in studies at hospitals in Stockholm and Oslo that investigated the use of DSCs to treat severe immune reactions, such as those that can occur after bone marrow or stem cell transplantation.
In 2014, one of Dr. Mattsson’s patients developed a severe immune reaction to his lungs and required total oxygen supplementation. After administration of DSC, the patient recovered rapidly. “We were actually able to discharge him within just a week and we avoided the ICU. I’ve always kept it in mind that these cells might actually be a treatment for this kind of acute respiratory distress syndrome,” says Dr. Mattsson.
When Dr. Mattsson saw that COVID-19 was causing similar respiratory failure, he knew it was time to test that hypothesis.
Visionary support for an unusual treatment
Through UHN support and a partnership with Ozmosis Research, the team developed a study aiming to answer three major questions: whether using DSCs to treat respiratory failure is possible, whether it’s safe and whether it’s effective. With so many unknowns, it was challenging to find an agency willing to provide funding.
“Unfortunately, because of the novelty, it’s considered a risk and people don’t like taking risks with their money. The risk-takers are visionary people who can see a good idea and go with it,” says Dr. Granton. Luckily, the team found that visionary support through philanthropy.
With funding secured, Dr. Mattsson reached out to his former colleagues Drs. Hanne Scholz and Yngvar Floisand in Oslo to see if they would be willing to provide the DSCs for this world-first study. They agreed.
The team worked through evenings and weekends to write the study protocol in only a few weeks instead of the normal multi-year development period. This was an incredible accomplishment considering that at the same time, the team was busy due to the pandemic itself.
Saving the sickest COVID-19 patients
The clinical trial, which is currently underway, is focused on patients who are critically ill with COVID-19 at three sites: Toronto General, Etobicoke General and Brampton Civic hospitals. All participants have acute respiratory distress syndrome and are in the ICU receiving supplementary oxygen.
The DSCs arrive from Oslo frozen. The team thaws and reanimates the cells before diluting them and injecting the solution into a patient’s veins on two occasions, two weeks apart. Throughout treatment, the team monitors the patient’s immune response.
Normally, the mortality rate of COVID-19 patients who are at such an advanced stage of the disease is 40 per cent. So far for the study participants, there have been no major adverse events and a zero per cent mortality rate. In fact, a significant number have been transferred out of the ICU and have even been discharged to rehabilitation or their homes.
“The patients are recovering from their acute illness and are going back to their previous lives. It’s a long road, a lot of rehab and but they’re on the road to recovery,” says Dr. Granton.
A brighter future for acute respiratory failure
To get a more accurate picture of DSCs’ impact, the team will need to compare patient outcomes to previous cases where patients did not receive this treatment. If the data demonstrates what Drs. Granton and Mattsson believe – that DSCs are effective in treating respiratory failure – they hope it will one day become a standard of care for COVID-19 and other causes of respiratory failure.
“Acute respiratory distress syndrome is not specific to COVID-19. This kind of severe lung reaction will be around after the pandemic,” says Dr. Mattsson.
This syndrome is one of the most common reasons for ICU admission and there is no specific treatment. Drs. Granton and Mattsson hope that their research can fill that gap. The outcome of this research study could help save lives long after the COVID-19 pandemic ends.